So we’ve reached the World Health Organisation’s recommended two years of breastfeeding.
Not deliberately – I didn’t set out to breastfeed for that long, and it happened more by error than it did by design – but either way, the question is, now what?
After two years of feeding the youngest day and night, and four months after deciding it’s time to stop nursing her, I still have absolutely no idea how to go about it, especially since she’s showing absolutely no signs of wanting to stop.
There’s a wealth of information out there when it comes to breastfeeding a newborn, but when it comes to feeding ‘older’ babies, there’s not so much.
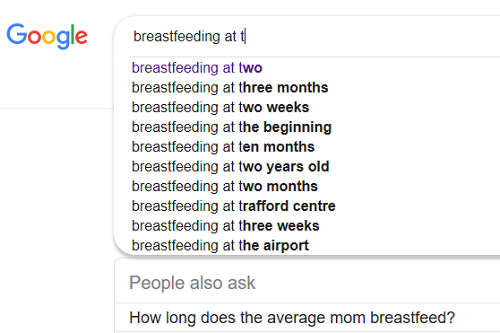
Put ‘breastfeeding at two’ into an internet search engine and it will automatically predict you’re searching for breastfeeding at two weeks or two months, not two years. And when you do hit on the age bracket you’re looking for, the information is generally from other mums based on their own experience, rather than professional experts.
Breastfeeding at two – now what?
At the time of writing (half term) the youngest is staying with grandparents for a few days in a bid to try and break the breastfeeding cycle, and when she gets back the milk bar will be officially closed. The thing is, though, I have no idea if that’s the right way to instigate weaning, what to do next or how to comfort her if she gets upset about it.
So, having shared my third breastfeeding journey as one of Medela’s #MedelaMums for the last two years, I put all my questions to Medela’s lactation consultant Sioned Hilton, and here’s what she said.
Is there a ‘right’ time to stop breastfeeding my baby?
“No, there is no right or wrong time to stop feeding – it is down to mum and baby’s preference,” Sioned says. “It is recommended that exclusive breastfeeding is up to six months, then introduce solids and to continue to breastfeed for as long as you both want. There are rare situations for medical reasons, such as certain medications (in the UK, HIV) where with a consultation from a health care professional around breastmilk, mums are informed of the risks and are able to make alternative choices,” she says.
How should I go about stopping breastfeeding my toddler?
“If your feeding patterns have gradually adapted as you return to work or your baby started nursery, you will have tailored your supply to meet these,” says Sioned. “For some mums it can be a planned gradual approach, others may need to stop feeding suddenly and need to manage their milk supply for comfort and down regulation. Some babies find this a time of uncertainty – they are used to having an awareness of mum’s presence, being there for a drink, meal, comfort or cuddles and this suddenly changes,” she says.
“If your toddler is old enough to understand that you wish to stop, you can use distraction – have a new cup and plate for meal times as a reward. If you always feed to assist her sleeping pattern, modify this whilst you are still feeding so that they don’t associate sleep with a breastfeed. It is useful to start with changing behaviour – offer water in a favourite cup or expressed milk, and plan an activity such as a walk or a ride in the car to change sleeping behaviours. If you co-room or co-sleep, you may want to start wearing pyjamas or a t-shirt so that access is a little more awkward. In the day, outfits that are less accessible, combined with distraction can delay a feed until it’s your choosing. Gradually dropping feeds and extending the time between these will help your body to down regulate supply.”
Should I offer my toddler an alternative to breast milk?
“This is a topical debate because we are subjected to so much influence that babies need follow on milk that is unnecessary,” says Sioned. “A healthy balance of food groups can meet your baby’s growing needs of protein, calcium and other essential minerals. Cow’s milk is suitable for toddlers over one year of age but it is important that they have full fat milk until the age of five. You can use cow’s milk, soya and almond milk for both drinking and cooking, and you can use expressed breastmilk if you have any in the freezer.”
How should I comfort her if she becomes distressed?
“If she can understand that you are no longer wanting to breastfeed you can talk to her – some mums say they no longer work, ‘broken’ or if you are pregnant that they are getting ready for the new baby. How you explain this is your choice,” advises Sioned. “Distraction always is a useful way to shift the focus – a new cup, an activity that you both enjoy, a ride in car, a bath and story at bedtime, a partner or family to settle and praise and rewards can also be used.”
How long will it take for my breast milk to ‘dry up’?
“This is a difficult one to predict,” Sioned says. “Some mums find that their milk drops significantly within one to two days of reducing frequency or when no longer night feeding. Other mums may find that it can take weeks and sometimes months to stop feeling leakage or milk present. If you have been feeding for a long period of time, think about how amazing this production line has been, and it is normal to expect down regulation of supply to take a while. This is why many mums gradually drop to morning and evening feeds, daily feeds and then see if they need to remove milk for comfort (just five minutes by hand so that you leave milk in the breast for the rise in feedback inhibitor enzymes to be at a level to stop the milk cell secreting milk.) If it takes longer than expected, you no longer feed or express and you experience milk leakage, it is important to have a chat with your GP. They will usually run some blood tests to measure your hormonal levels.”
Do I need to worry about getting mastitis at this stage?
“There is a potential risk of mastitis at any stage when there is milk in the breast and you experience engorgement, and this is something to have an awareness of as you down regulate supply,” says Sioned. “This is usually inflammatory mastitis and treatment is to relieve the engorgement, increase frequency and drain milk from the breast to comfort, rest recuperate and if necessary, take pain relief. Seek advice within 24 hours if it is not resolving. If you know you are prone to mastitis you may need to take things slower.”
Is there anything else I should bear in mind?
“Your toddler is growing at a rate that changes day to day. Some days she will be busy exploring and not feed, other days when she is teething, under the weather or tired may see her feeding more,” Sioned says. “If there is a sudden change in routine, it can be unfamiliar and unsettling – whilst a holiday or days away may be a distraction and help for others, it may be too much. As they take more family meals, many toddlers naturally down regulate and take less, but feed often. They are experts at power snacking and those lazy chilled feeds, so just take it a day at a time. Have the support of family and friends to help out too. As you start to wean off breastfeeding, you will start ovulating again, you can become pregnant and your periods may return. Some mums tell us that their babies are fussier when they are on their period, but this is anecdotal. You can tandem feed a toddler and newborn – so if you are pregnant and feel that you should stop, there is no reason to. Your supply adapts as a result of the pregnancy hormones, and you may find your breasts/nipples are more tender or your toddler is a little fussier as your supply adapts.”
And the million-dollar question: will my previously equal-sized boobies return to their once equal size, or will one stay blown out of all proportion to the other for the rest of eternity?
“Often one breast has a larger storage capacity and baby may have a preference to one breast. It could be volume, flow or just a preference,” explains Sioned. “When you breastfeed and lactate the breasts become a functioning organ. The cells and breast tissue require oxygen and nutrition and use a lot of energy manufacturing milk and moving its production from the milk sacs to the nipple. It is understandable that the breasts tone and become very efficient, and occasionally mums may see a difference in breast size. Asymmetrical breasts are normal from puberty onwards but when lactating it may be more visible.”
“After breastfeeding stops the breasts then only change with the menstruating cycle. If mum maintains a healthy weight the breasts will have a modest subcutaneous, interstitial level of fat whilst ladies with a higher body mass index may have a higher ratio fuller bust. A good padded bra may be the answer for a few months.”
I’m not entirely sure whether the answer to the last question is yes or no, but I guess time will tell! I do hope this post has been useful to breastfeeding mamas out there – whether you’ve been doing it for two weeks, two months, or two years, from the youngest and I – good luck!































I never managed to get established with breast feeding any of my three children, although I really wanted to , I often wonder if the help that is available now had been then, would it have made a difference #thatfridaylinky@_karendennis
Good post! I stopped at 12 months with my eldest because I was pregnant again and I stopped at 16 months for my youngest. I think I had a harder time coping with it than they did but they both seemed to do well during the transition periods where I offered them sippy cups and only nursed during naps or night time.
Never an easy decision on when to top breastfeeding the kids. With the influx of alternatives to breastfeeding these days, it may seem easy to switch to them, but no one really cares if they have any effect in the long run on our kids
This is great advice, in an area not often talked about. I breastfed one of my girl’s until she was around 18 months old. It wasn’t my initial intention but just happened and we were both comfortable and happy about it. It was only when I decided that it was time to stop that I realised how difficult both the decision and what to do was. But then we had a mini break, a few days away from home. For the first time she slept in a different room (in a caravan) and didn’t even ask for her nightly feed. We were so busy in the daytime she didn’t ask for feeds either. When we got home the first things she did was ask for milk, but I just told her that it had gone away and she was fine. She never asked again.
#mmbc
While I may not be armed with the correct equipment to require this post. It was really interesting and full of great advice! I will be certainly be sharing it with my Mummy friends. #ItsOK
I think one of the reasons I stopped feeding at 13 months was I suspected it would be harder to do when they were toddlers, glad to see some advice about it. #itsok
Some excellent advice here Natalie xx #ItsOK
Some fab advice there and I hope things work out well for you both over the coming weeks if you do decide to stop. I like the idea of reducing feeds slowly. It’s a hard connection to break when it’s been so natural and part of the every day for so long. Thanks for joining us for the #dreamteam xx
Thanks for sharing this with us at #itsok, it’s such valuable information. There’s plenty on the Internet about bf babies but practically nothing for bf older babies, so this was a great read. Good luck with your onward journey!
Good advice #KCACOLS
Fab post and really.helpful for someone breastfeeding X #kcacols
Congratulations on breast feeding for so long. I hope that weaning her off is easy for both of you. Loads of useful information here. #KCACOLS
Brilliant advice. And well done on making it to 2 years! Thanks so much for linking up at #KCACOLS. Hope you come back again next time!
Fantastic advice, really accessible and thank you for doing the research that is lacking out there. #KCACOLS
This came at a great time. I am, actually, still nursing my almost 3-year-old. He will be 3 in May. I just can’t get myself mentally ready to wean, and he doesn’t seem ready either. It is still such a sweet moment for us. But my family and my husbands family give me crap over it all the time and it really bothers me. It is hard to do something that still feels so right and get no support for it. Thanks for this post. #KCACOLS
Great that you’re writing about this, and with a lot of helpful advice as well. It’s sad that there still seems to be some ‘shame’ attached to breastfeeding toddlers. If mother and child are both comfortable with it, they shouldn’t have to feel embarrased xx #KCACOLS
I hope it goes well for you and isn’t too stressful for either you or your bub. #kcacols